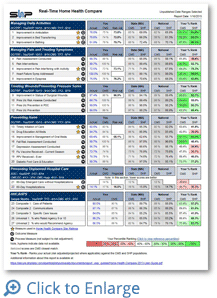
With CMS’s proposed Five-Star quality rating system, overall quality will be depicted as one score, ranging from one to five stars. Ten of the twenty-seven HHC quality measures will be the basis for this scoring. How you are performing today will be used in the calculations for your star rating as it begins later in CY15.
With Value Based Purchasing (VBP) on the horizon, it is not much of a leap to believe that soon CMS will consider something like five-star in their payment penalties/bonuses. The five-star rating system presents another threat if you don’t deliver quality care, or conversely, an opportunity if you do.
The five-star rating system is currently used to rank nursing homes, Medicare Advantage plans and physician groups. In 2015, Medicare Advantage plans that score a 4 or 5 star will receive quality bonus payments. With their 3 year lag between activity and payment, this means that 3.5 star plans that did not improve in 2012 will take a pretty hefty payment cut in 2015.
One of my previous blogs from 2014, “Man Cannot Live by OASIS Edits Alone”, urges managers to go beyond “OASIS scrubbing” and to invest in the next generation solution for survival – a solid performance improvement system. Now there’s a direct return on the quality of care investment.
Using FY13 data, CMS reports over 50% of home health agencies will be reported with 3 stars and only 2% of the agencies with a rating of 5 stars. It’s a New Year and a great time to get a solid handle on the 10 reported metrics below that will be used in the five-star rating (we believe that HHCAHPS scores will eventually be included). Getting into the coveted top quintile for each measure will help insure your success.
Process Measures
- Timely Initiation of Care
- Drug Education on all Medications Provided to Patient/Caregiver
- Influenza Immunization Received for Current Flu Season
- Pneumococcal Vaccine Ever Received
Outcome Measures
- Improvement in Ambulation
- Improvement in Bed Transferring
- Improvement in Bathing
- Improvement in Pain Interfering With Activity
- Improvement in Dyspnea
- Acute Care Hospitalization