Home Health Final Rule confirms Home Health Value-Based Purchasing (HHVBP) as proposed
CMS issued the Final CY 2017 Home Health PPS Rate Update in the Federal Register on November 3rd. All of the proposals to update the VBP program were finalized with no changes regardless of stakeholder comments. The one change that no one argued was to eliminate 4 of the 21 VBP measures:
- Care Management: Types and Sources of Assistance;
- Prior Functioning ADL/IADL;
- Influenza Vaccine Data Collection Period;
- Reason Pneumococcal Vaccine Not Received
Seemed obvious, but it was nice to get the confirmation that CMS agreed that some of the selected measures were either duplicative or not well defined in the CY 2016 Home Health Prospective Payment System (PPS) final rule.
One of the commenters did resurrect the issue of whether Medicare PPS payments should be adjusted based on “non-Medicare” (Medicaid, Medicaid HMO, Medicare Advantage) clinical outcomes. Although the claims-based measures are for Traditional Medicare patients only, the HHCAHPS and OASIS-based measures reflect outcomes for all Medicare and Medicaid episodes.
Below is a chart of SHP outcomes from our national database for all Medicare/Medicaid payers (as posted in Home Health Compare – HHC) compared to Traditional Medicaid and Medicaid HMO only. Every Medicaid outcome is below the Home Health Compare payers with one exception, Improvement in Oral Medications.
| Measure | HHC Payers | Medicaid | Difference |
|---|---|---|---|
| Improvement in Ambulation | 72.8% | 70.1% | -2.7% |
| Improvement in Bathing | 75.3% | 73.7% | -1.6% |
| Improvement in Bed Transferring | 70.1% | 67.9% | -2.2% |
| Improvement in Dyspnea | 74.3% | 71.2% | -3.1% |
| Improvement in Management of Oral Medications | 62.7% | 66.3% | 3.6% |
| Improvement in Pain Interfering with Activity | 73.9% | 68.6% | -5.3% |
| Drug Education on All Medications Provided to Patient/Caregiver | 97.5% | 97.1% | -0.4% |
| Discharge to Community (not risk adjusted) | 72.3% | 69.6% | -2.7% |
| Infuenza Immunization Received for Current Flu Season | 77.5% | 66.7% | -10.8% |
| Pneumococcal Polysaccharide Vaccine Ever Received | 80.9% | 68.6% | -12.3% |
| Care of Patients (HHCAHPS) | 89.2% | 85.9% | -3.3% |
| Communications between Providers and Patients (HHCAHPS) | 86.6% | 84.7% | -1.9% |
| Specific Care Issues (HHCAHPS) | 85.9% | 85.5% | -0.4% |
| Overall Rating of Home Health Care (HHCAHPS) | 84.2% | 80.3% | -3.9% |
| Willingness to Recommend the Agency (HHCAHPS) | 79.8% | 76.4% | -3.4% |
CMS did note in the proposed rule that “The NQF is currently undertaking a 2-year trial period in which new measures and measures undergoing maintenance review will be assessed to determine if risk-adjusting for sociodemographic factors is appropriate.” Until then, agencies with a higher proportion of Medicaid patients will likely be disadvantaged.
One notable change in the final rule was regarding the case-mix variable point changes and the recalibrated case weights. With the final rule, the case-mix weights changed dramatically. Comparing to the CY17 proposed rule case-mix weights, all but 5 of the case-mix weights for the 153 HHRGs decreased. Case-mix weights decreased by an average of over 2.7% overall. Since CMS recalibrations are required to be budget neutral, an adjustment factor of 2.14% will be added to the national episodic rate to reflect these case-mix decreases. Remember this when you are looking at your January 2017 case-mix weight reports compared to December 2016, where a decrease of over 2% will likely accompany this change.
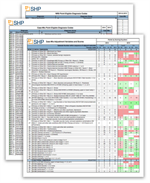
To help agencies visualize the 2017 Final Rule case-mix changes, SHP has prepared a PPS and NRS Point Scoring 2014 - 2017 Comparison Guide to demonstrate how the HHRG scoring is affected, including the mapping and scoring of the new clinical and functional domains.
Given that agencies in each of the 9 VBP states are competing against each other, providers must not only improve their outcomes to generate higher Total Performance Scores (TPS), but also improve more than their competition in order to increase the opportunity for higher bonus adjustments under VBP. Benchmarking your scores to determine your relative position within your state will be very important in tracking your progress.
Join Zeb Clayton and me on December 14th, 2016 for a HHVBP webinar where we'll share the latest insights on VBP, including outcome measure trends and a new report we created to help agencies see how their TPS scores compare to others. Registration is open!