CMS Home Health Proposed Rule shares PDGM winners and losers
In the CY 2019 Home Health Proposed Rule, CMS shared a level of detail not seen before – an agency specific list of how agencies will fare under the changes they are proposing. Wow. CMS shared the agency revenue impacts of the Patient-Driven Groupings Model (PDGM) versus the current 153-group PPS reimbursement revenue. The range of the revenue impact is quite wide. For agencies with at least 20 payment episodes, the impact ranged from a 51.5% decrease in revenue to a 67.3% increase in revenue.
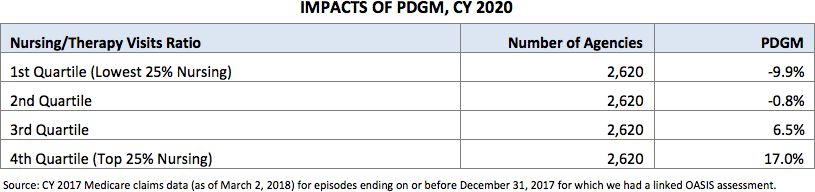
Based on the chart below (HH Proposed Rule p. 525) in the rule, it is clear a significant reason for this reimbursement variation is due to agencies with a higher percent of therapy visits and cases. CMS shared a ratio of nursing to therapy visits across the four quartiles of the reported agencies. Under the proposed rule, CMS has removed therapy visit thresholds as a factor in assigning case mix weight. The recalibrating of the case weights based on patient characteristics have significantly changed the reimbursement on therapy cases.
I have heard some agencies question the accuracy of these numbers since they felt the number of episodes reported looked low. Keep in mind that, since CMS was looking at claims data as of March 2nd, many of the episodes that were completed near the end of the year may not yet have been paid. In addition, as with the original Home Health groupings Model (HHGM) proposed rule, CMS has identified many primary diagnosis codes that would not be “appropriate” to be covered by home health.
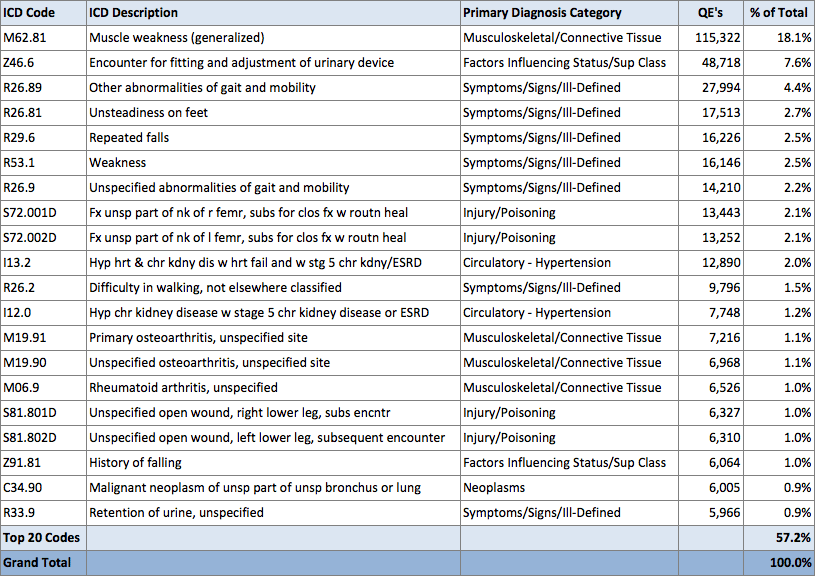
Where CMS described these as Questionable Encounters (QEs) under HHGM, CMS is only listing about 38,409 codes in their PDGM Grouper Tool that would be eligible. If the primary code does not match this list, CMS will not be able to assign the 30-day period to one of the six PDGM clinical groups, and will likely return the claim to the provider to be recoded.
Looking at the SHP national database for CY 2017, about 17% of the 3.6MM payment episodes in our database had a primary diagnosis code that would be considered a QE under PDGM. CMS did add 8 diagnosis codes that were considered a QE under HHGM, with Urinary Tract Infection being the most frequently used. About 60% of the QE codes are in the top 20 primary diagnosis codes found in the SHP national database, as illustrated by the chart below. I would recommend reviewing your top questionable diagnoses and educating your staff as to more appropriate coding in preparation for these upcoming changes.