The Hospice Quality Reporting Program (HQRP) Star Ratings are Coming!
 The Centers for Medicare and Medicaid Services (CMS) released their annual Hospice Wage and Payment Rate proposed rule for FY 2022 in the Federal Register on April 14 and there was plenty of updates regarding the HQRP. Many were expected but the one I found noteworthy is the addition of public reporting for a new CAHPS Hospice Survey Star Rating.
The Centers for Medicare and Medicaid Services (CMS) released their annual Hospice Wage and Payment Rate proposed rule for FY 2022 in the Federal Register on April 14 and there was plenty of updates regarding the HQRP. Many were expected but the one I found noteworthy is the addition of public reporting for a new CAHPS Hospice Survey Star Rating.
While adding Star Ratings has been mentioned in the past, it was not on my radar given the fact CMS had previously announced plans to add a new Hospice Care Index (HCI) and replace the Hospice Visits when Death is Imminent Measure Pair with the Hospice Visits in the Last Days of Life measure. Both had been part of a CMS request for comment that was outside of the normal hospice rule-making that I blogged about last fall.
CMS notes the stars would range from one star (worst) to five stars (best) and be calculated based on “top-box” scores for each of the eight CAHPS Hospice Survey measures. A hospice-level score for a given survey item would then be calculated as the average of the individual-level responses, with adjustment for differences in case mix and mode of survey administration.
Providing a simpler way to share Caregiver Experiences using a Star Rating is a reasonable goal. It is confusing to review the current eight measures and composites on Care Compare and interpret what may be most important to consider when selecting a Hospice. Star rating simplifies the review and according to CMS, it will “benefit the public in that they can be easier for some to understand than absolute measure scores, and they make comparisons between hospices more straightforward.”
What is concerning is that CMS plans to use a similar approach to other CAHPS programs to calculate the star rating cut-points using statistical clustering. This design intends to minimize the score differences within a star category and maximize the differences across star categories. It sounds reasonable but under the Home Health CAHPS program (HHCAHPS), the reporting of star ratings has been very uneven.
For example, in the last 5 years, the quarterly posting of the percent of “5” Star rated home health agencies has fluctuated considerably (see chart).
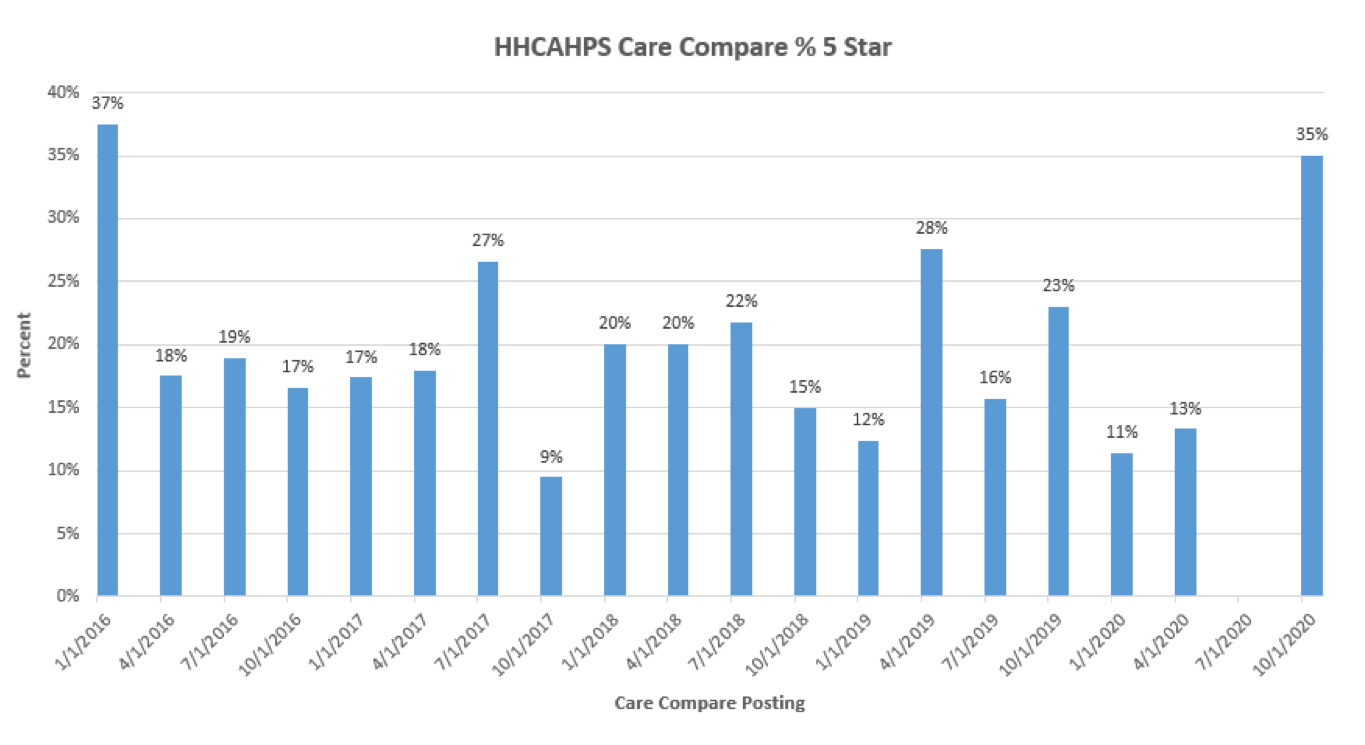
It doesn’t seem logical that the 12 month rolling average of scores would show one quarter with 37% of providers achieving a 5 star rating, followed by a quarter in which the percentage of 5 star providers would be cut in half or more!
In the proposed rule CMS does add a couple of changes to the approach they claim will promote more stability of the cut-points. CMS describes a two-stage approach as follows:
- Stage One: Determine initial cut-points by calculating the clustering algorithm among hospices with 30 or more completed surveys over 2 quarters (that is, 6 months); restricting these calculations to hospices that meet a minimum sample size promotes stability of cut-points.
- Stage Two: Compare mean measure scores for the bigger hospices used in the first stage to all other hospices, and update cut-points by adjusting the initial cut-points to reflect the normalized difference between bigger and smaller hospices.
Each Hospice would be assigned an overall CAHPS Hospice Survey Star Rating by averaging the star ratings across the 8 measures, using a weight of ½ for Rating of the Hospice, a weight of ½ for Willingness to Recommend the Hospice, and a weight of 1 for each of the other measures, and then rounding to a whole number. Hospices would need a minimum of 75 completed surveys in order to be assigned a Star Rating.
Let’s hope this newer two stage approach helps to limit the wide swings in ratings we have seen with HHCAHPS in the past. We should expect to see CMS webinars on the calculations and approach to the new CAHPS Hospice Survey Star Rating once the rule is finalized for implementation in FY 2022. However, don’t wait to identify your problem areas and improve your CAHPS scores. With a rolling 8 quarters of data, your CAHPS Hospice surveys this quarter will be part of your star ratings for well over a year if they begin posting on Care Compare as expected next May.

