Are Recerts Biting Into Your Bottom Line?
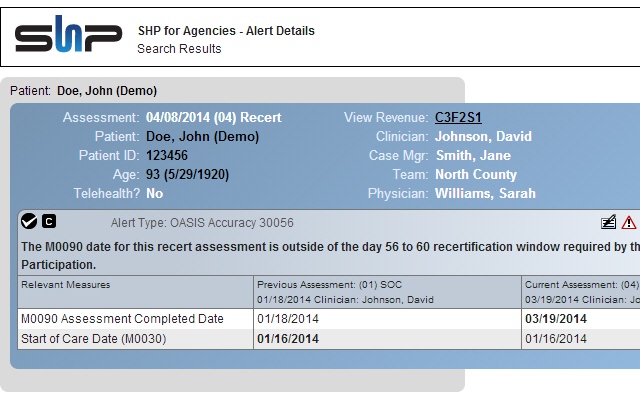
CMS expects Recertifications (recerts) to be completed within the last five days of a payment episode (days 56 to 60), although they’ll accept late submissions under legitimate circumstances. The state also generates a warning upon receipt of a recert completed on day 62 or later, and SHP also alerts clients, but despite these double warnings, late recerts continue to be an issue.
Why is this important and what can you do to correct the situation?
Why it’s important:
- Failure to submit recerts on a timely basis is a violation of the Conditions of Participation, and that’s never a good thing.
- Late submissions increase your paperwork burden and drive up labor costs as you must create additional documentation to explain the delay.
- The longer it takes to submit the RAP, the longer it takes to get paid.
- If you have an aggressive surveyor, you’ll have an issue.
- CMS may eventually initiate a penalty, so getting this under control now is advisable.
What you can do:
- Conduct regular case management conferences. If your agency regularly conducts these, then you’re less likely to have a problem.
- At the very least, print out a weekly recert list and assign someone the responsibility of reviewing it religiously. With thinning margins, extra work and delayed payments are to be avoided at all costs (no pun intended).
