OASIS-E1 Instrument is Released with Little Fanfare

In the first week of January 2024, CMS quietly announced the release of the latest draft of OASIS version E1. The subdued announcement can be attributed to the limited updates planned for the tool, set to take effect on January 1, 2025. CMS has mentioned that the accompanying OASIS-E1 manual will be made available at a later date.
Beginning in CY 2025, agencies must start collecting OASIS data for all patients, irrespective of their payer source. In the CY 2023 final rule, CMS emphasized the importance of capturing the most accurate representation of care quality by utilizing assessment-based measure rates derived from OASIS data submitted for all HHA patients receiving skilled care, regardless of payer.
To facilitate a smooth transition, CMS will implement a phase-in for patient assessments discharged between January 1, 2025, and June 30, 2025, with mandatory participation starting from July 1, 2025. Exemptions will continue for patients under 18 or those receiving only maternity or personal care.
The E-1 changes encompass:
- Adding a new item (O0350) for the new HH QRP COVID-19 Vaccine measure that was finalized in the CY 2024 rule-making
- Removing of OASIS items deemed no longer necessary:
- M0110 – Episode Timing
- M2220 – Therapy Needs
- GG0130 and GG0170 – Discharge Goal
The changes are very minor in comparison to the updates made between OASIS-D1 and OASIS-E. Although the changes with OASIS-E were significant, most providers I spoke with were more matter-of-fact about the implementation. Many were well-prepared, having trained their staff in advance for the changes that took effect January 1, 2023. One even compared it to Y2K, essentially a non-event.
With one year under OASIS-E completed, I reviewed how the new Transfer of Health (TOH) process measure scores were trending. The new TOH to Providers and Patients measures are part of the cross-setting Post-Acute Care (PAC) measures introduced with OASIS-E. The measures calculate how often the home health agency provided a current reconciled medication list to providers and patients at transfer and/or at discharge. CMS plans to publicly report these two measures on Care Compare as of the January 2025 refresh onwards.
As expected, these scores are improving each of the first four quarters during CY 2023 as reflected in the SHP National Database.
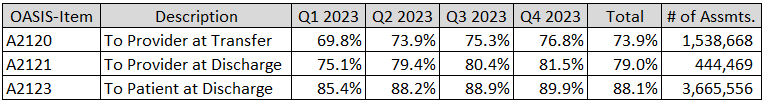
CMS will consolidate A2120 and A2121 scores as an overall provider TOH score. To ensure score reliability, agencies must have a minimum of 20 eligible cases per quarter for the measure to be reported. Otherwise, a footnote will indicate that the number of quality episodes is too small for reporting.
Out of curiosity, I compared how agencies reported the different ways they provide the TOH information to providers and patients.
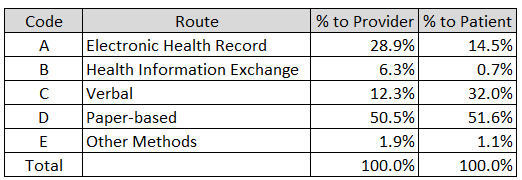
The percentages include entries that are for more than one route (i.e. check all that apply). As one example:
If a patient receives a paper copy of their medication list, receives education about their medications by the home health nurse at discharge, and is notified that the home health patient portal is another means that the patient can obtain their discharge medication list, the route would be coded as an A, C and D.
Agencies have until the end of Q1 2024 to enhance TOH scores for the upcoming Care Compare release. It is advisable for agencies to assess their current scores and validate that their workflows accurately capture these new process measures.

