PDGM recalibrates revenues in budget neutral manner
Now that we know the Patient-Driven Groupings Model (PDGM) will officially start January 1, 2020, it’s time to dig a little deeper into understanding how the case-mix weights of the 432 PDGM groups were established. The first premise to note is that CMS’ mandate was to create PDGM in a budget neutral manner. It is this concept of recalibrating, or redistributing, revenues that is necessary to ensure that total Medicare outlays are the same under PDGM as are paid today.
Of course, the “neutral” part assumes your agency provides care similar to the national average. It is the dynamic of the differences in each agency’s patient mix and visit utilization that sets the stage for winners and losers under PDGM. Based on recent CMS data on agency impacts, the top decile of agencies benefiting under PDGM will see their revenues increase by an average of 33.5%. The lowest decile will see a decrease in revenue of 20.2% on average (this analysis included agencies with at least 20 completed episodes).
The second important premise to understand is that, in creating the case-mix weights, CMS uses an estimate of resource use or cost based on historical visit utilization. Yes, they use visit data from how agencies have been practicing care. The visit data for PDGM was based on agency CY 2017 home health claims.
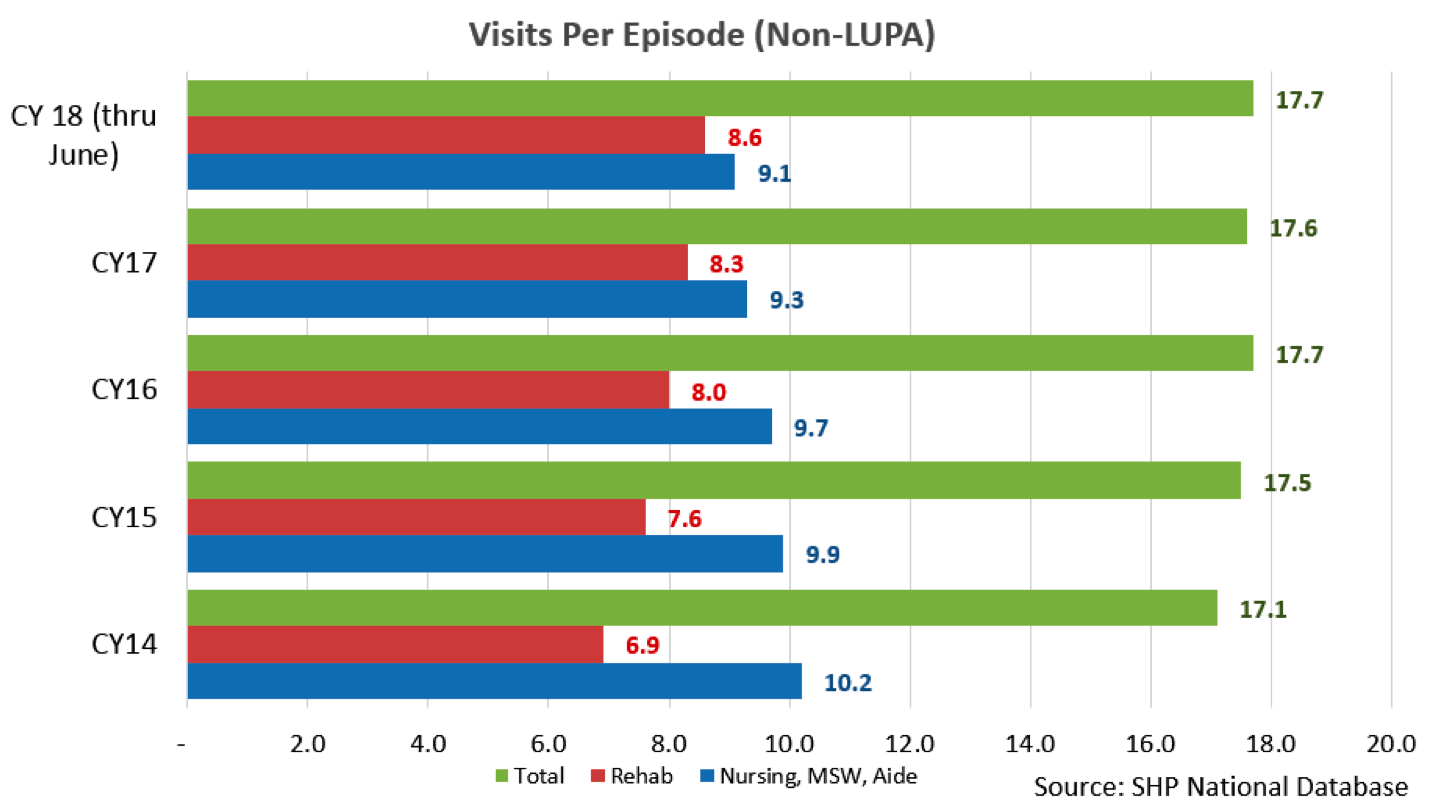
In the proposed rule, CMS noted how agency practice reflected increasing therapy visit utilization. Using data from the SHP database, the national averages for rehab visits (physical, occupational and speech therapy) have steadily risen over time. Even though overall visits per episode have flattened out, therapy visits have continued to increase, which was offset by the decreasing visit counts for nursing, social work and aide services (see chart).
Under the current HH PPS reimbursement system, the 153 HHRG case-mix weights are recalibrated every year. The annual changes are relatively minor as they are adjusting to the four–equation model (i.e. 0-13, 14+ therapy visits) using therapy visits as the foundation. Under PDGM, CMS is no longer allowed to use therapy visits as a case-mix factor, so the change is like a “do-over”. The model realigns case-mix weights and the associated revenues on historical resource use or costs modeled on the newly established PDGM components and groupings. The revenue from the more profitable therapy cases are being redistributed to the lower paying complex care nursing cases.
Additionally, starting in CY 2020, CMS will be using a discipline-specific cost-per-minute factor plus non-supplies from cost reports in determining resource use. Although controversial, it is different from the weighted minutes-of-care that uses the CY 2016 Bureau of Labor Statistics for the CY 2019 rates. This suggests how important accurate annual cost reporting will continue to be.
Since PDGM won’t start for another year, CMS will again recalibrate the case-mix weights using the latest available claims data from CY 2018 prior to implementation. Home health agencies will not know the final weights until the final rule is published next October. What should we expect? Likely not a significant change from what was posted in the Oct 2018 final rule. This is in part due to the fact that agencies have not yet changed practices for PDGM, especially since the incentives to provide therapy at higher levels is still a revenue driver under the current reimbursement system.
I also would not expect utilization to change significantly in CY 2019. It will not be until the final rule for CY 2022 (using claims data from CY 2020) that we will likely see more significant changes in case-mix weights. This will be due to the visit utilization related operational changes agencies will likely make under the new reality of PDGM.

