OASIS-E is delayed due to COVID-19
Last week, the Centers for Medicare and Medicaid Services (CMS) announced in their Interim Final with Comment Rule a delay in the implementation of OASIS-E which was slated to begin on January 1, 2021. This is good news for Home Health Agencies (HHAs) that have been consumed with the impact of COVID-19 as part of the Public Health Emergency (PHE).
CMS noted they would “require HHAs to begin collecting data on the SPADEs beginning with the start of care, resumption of care, and discharges (except for the hearing, vision, race, and ethnicity SPADEs, which would be collected at the start of care only) on January 1st of the year that is at least 1 full calendar year after the end of the COVID-19 PHE.” For example, if the COVID-19 PHE ends on September 25, 2020, the collection of OASIS-E data elements would start on January 1, 2022.
As I noted in a recent blog, the magnitude of changes in adding the new Standardized Patient Assessment Data Elements (SPADEs) would require a massive training effort of agency staff as well as a large investment by their software and technology vendors. CMS is providing these needed flexibilities for HHAs to have more time to respond effectively to the serious public health threats posed by the spread of COVID-19.
Under the PHE, HHAs have been faced with incredible challenges in maintaining staffing levels, securing personal protection equipment (PPE), and dealing with decreasing admissions. Cash flow has been seriously impacted. One consequence of these staffing limitations and patients refusing care is HHAs have seen their PDGM LUPA rates dramatically increase.
For 30-day payment periods beginning in the first three months of CY 2020, the table below shows that LUPA rates have increased more than 50% between January and March, both nationally and in some sample states. Early April data shows this continued increasing trend.
| Data Set | Jan '20 | Feb '20 | Mar '20 |
|---|---|---|---|
| National | 7.8% | 9.0% | 12.5% |
| New York | 9.2% | 11.2% | 16.5% |
| New Jersey | 11.7% | 12.1% | 17.8% |
| Louisiana | 4.8% | 5.5% | 7.5% |
| Texas | 5.5% | 6.1% | 9.6% |
| Florida | 6.9% | 8.7% | 11.2% |
With the addition of a new ICD-10 code for COVID-19, SHP is tracking patients with U07.1 under a new diagnosis category. Tracking metrics and measures in our reporting for patients with a primary diagnosis of COVID-19 with provide insights in helping HHAs manage this population. There is no surprise that the volume of these cases are climbing, as hospitals have been referring patients back home as COVID-19 hospitalizations have peaked in many states.
Across all payers within our SHP national database, the April 2020 SOC/ROCs with COVID-19 as a primary diagnosis is climbing sharply (see graph).
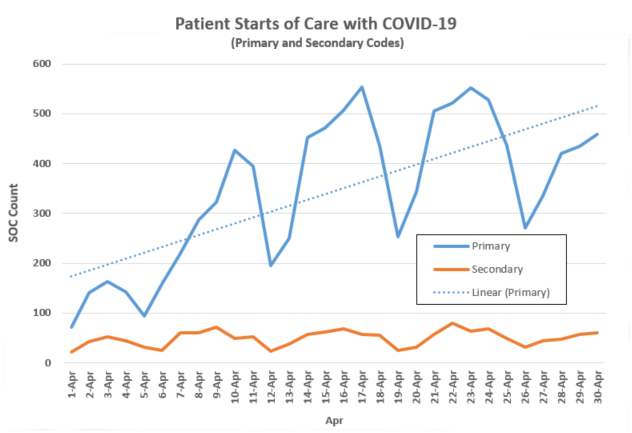
A review of the ~12,000 patients with COVID-19, shows that over 90% of have been admitted from an institution setting. Although under PDGM, the case-mix weight for institutional admissions is higher, a closer look at these claims to determine the LUPA rates will be warranted. We will continue to track these rates in the next few months.
As part of our commitment to help your HHAs manage PDGM under this pandemic, please join BKD’s Mark Sharp and Aaron Little during our Wednesday Winning Webinar on May 13th as they share insights in assessing the impact of COVID-19 and PDGM on operations and cash flow.

